Procedures
Endodontic Surgery
Why would I need endodontic surgery?
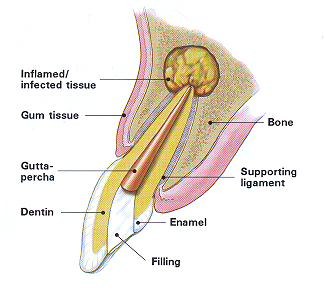
Surgery can help save your tooth in a variety of situations.
- Surgery may be used in diagnosis. If you have persistent symptoms but no problems appear on your x-ray, your tooth may have a tiny fracture or canal that could not be detected during non-surgical treatment. In such a case, surgery allows your endodontist to examine the root of your tooth, find the problem, and provide treatment.
- Sometimes calcium deposits make a canal too narrow for the cleaning and shaping instruments used in non-surgical root canal treatment to reach the end of the root. If your tooth has this “calcification,” your endodontist may perform surgery to clean and seal the remainder of the canal.
- Usually, a tooth that has undergone a root canal can last the rest of your life, and never need further endodontic treatment. However, in a few cases, a tooth may fail to heal. The tooth may become painful or diseased months or even years after successful treatment. If this is true for you, surgery may help save your tooth.
- Surgery may also be performed to treat damaged root surfaces or surrounding bone.
Although there are many surgical procedures that can be performed to save a tooth, the most common is called apicoectomy or root-end resection. When inflammation or infection persists in the bony area around the end of your tooth after a root canal procedure, your endodontist may have to perform an apicoectomy.
What is an apicoectomy?
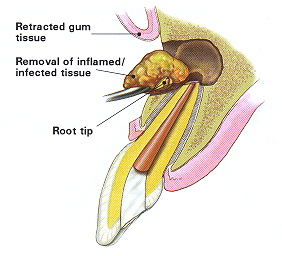
In this procedure, the endodontist opens the gum tissue near the tooth to see the underlying bone and to remove any inflamed or infected tissue. The very end of the root is also removed.
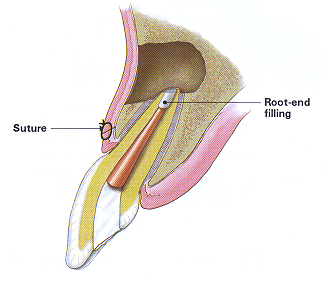
A small filling may also be placed to seal the end of the oral canal, and a few stitches or sutures are placed in the gum to help the tissue heal properly.
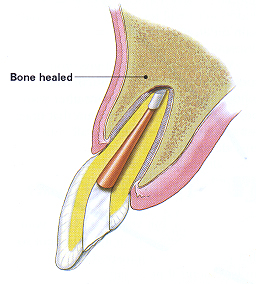
Over a period of months, the bone heals around the end of the root.
Are there any other types of endodontic surgery?
Other surgeries endodontists might perform include dividing a tooth in half, repairing an injured root, or even removing one or more roots. Your endodontist will be happy to discuss the specific type of surgery your tooth requires.
In very complex cases, a procedure called intentional replantation may be performed. In this procedure, a tooth is extracted, treated with an endodontic procedure while it is out of the mouth, and then replaced in its socket.
The procedures are designed to help you save your tooth.
How do I know the surgery will be successful?
Your dentist or endodontist is suggesting endododontic surgery because he or she believes it is the best option for you. Of course, there are no guarantees with any surgical procedure. Your endodontist will discuss your chances for success so that you can make an informed decision.
What are the alternatives to endodontic surgery?
Often, the only alternative to surgery is extraction of the tooth. The extracted tooth must then be replaced with an implant, bridge, or removable partial denture to restore chewing function and to prevent adjacent teeth from shifting. Because these alternatives require surgery or dental procedures on adjacent healthy teeth, endodontic surgery is usually the most cost-effective option for maintaining your oral health.
No matter how effective modern tooth replacements are – and they can be very effective – nothing is as good as a natural tooth. You’ve already made the investment in saving your tooth. The pay-off for choosing endodontic surgery could be a healthy, functioning natural tooth for the rest of your life.
Surgical Appointments
The following is an explanation of what typically happens at surgery appointments. Please note that each patient is different and treatment may vary.
Surgery Consultation: This appointment is required before all surgeries are scheduled. During this visit an examination of your x-ray along with the tooth in question is completed. If you are traveling from out of town, this visit may be replaced with a phone consultation once we have received x-rays of your tooth from your family dentist. To prepare you for your surgical procedure, an in-depth explanation of what to expect before and after the procedure is provided. All medical/health concerns will be addressed at this time. If you take aspirin or coumadin daily, you should inform the doctor who will be treating you. In addition, a step-by-step discussion of the surgical procedure will be given with illustrations from our surgical pamphlet. This appointment takes approximately 30 minutes and its focus is to make sure all of your questions are answered. At the end of this visit, you will be given an information packet which reviews the consultation discussion. You will also be given prescriptions. The morning of the surgery you will need to eat a good breakfast and start all of your prescribed medications. Before leaving your consultation, the cost for your surgery will be estimated and you will be given the opportunity to schedule an appointment with the receptionist. Keep in mind that a driver should accompany you at the time of your surgery. You are strongly advised not to drive yourself home after your surgery so if you need to make arrangements for a driver, you may call us at a later time to set up your appointment.
The Surgical Procedure: You will be scheduled for a 1 to 2 hour appointment for the day of your surgery. The procedure typically takes 30 to 45 minutes. The remainder of the scheduled time is to be used for allowing the surgical site to numb (15-30 minutes), and to review the post-surgical instructions.
The following is an overview of the surgical steps:
- Local anesthetic is given
- The surgical site is incised, the gums are reflected to see the underlying bone
- Removal of inflamed or infected tissue around root end
- Removal of the root end
- A small filling is placed to seal the end of the root canal
- Examination of root structure for cracks or splits
- Gum tissue is placed back to position and sutures are placed
- Gum dressing may be placed over the wound if needed
- Final x-ray is taken (this x-ray will be sent to your family dentist with a letter)
- An ice pack is applied to surgical area
After your surgery it is advised that you are escorted home by your designated driver. Once home, try to get as much rest as possible for the remainder of the day and the following day. Please see the “Post Surgical Instructions” for medication instructions and care of surgical site.
What Symptoms To Expect After The Surgery:
- Inflammation of the tissue around the surgery site
- Slight bleeding for the first 24 hours
- Some swelling for the first 24-48 hours
- Some bruising and discoloration of the tissue near the surgery site
- Some bruising of the cheek around the surgery site (usually in farer complications)
- Anesthetic numbness 4-6 hours after procedure
- Paresthesia: is a risk when performing surgery, however is very rare. Paresthesia means numbness which can occur in the jaw, tongue or lip area following root canal surgery. Please discuss this with your doctor if you have any questions.
Note that all of these symptoms can be reduced by icing the surgical area after treatment.
Post Surgical Appointment: Any remaining sutures will be removed at this visit. An examination of the tissues at the surgery site is completed.
Recall Appointment: One year after the completion of your endodontic treatment, our office will send you a post-card asking you to come in for a check up. Occasionally patients will be asked to come in for recall appointments in less than one year. There is no charge for this appointment. It is a 10 minute visit for us to take a new x-ray of the surgical site and re-confirm that the site is healing appropriately. This x-ray will be sent to your family dentist with a letter.
Post Surgical Instructions
- Rest: After your surgical treatment go directly home and rest as much as possible for the remainder of the day and the day after. Your discomfort should be minimal after the first 12 hours.
- Medications: Continue to take your medications as prescribed.
- Antibiotic:Continue to take your antibiotics every six hours until gone.
- Pain Medication: Continue taking your pain medication every 4-6 hours as needed for two to three days after surgery.
- Ice: Continue icing (15 minutes on; 15 minutes off: etc.) for the first 6-8 hours after surgery, or until you go to bed.
- Elevate: When you lie down, keep your head elevated with an extra pillow for the first 48 hours
- Do Not: Do not blow your nose. You may cause unnecessary swelling. Do not raise your lip to look at the sutures. This may disrupt or tear the sutures.
- Eating: Eat what is comfortable to you. Try to avoid eating very hot, spicy or brittle, crunchy foods and liquids. Avoid hard foods that require heavy pressure to chew. Do not drink fluids through a straw.
- Swelling, Discoloration and Bleeding: Some swelling should be expected up to 48 hours after surgical treatment. Do not be alarmed if you develop swelling. Swelling is a normal occurrence caused by working with the tissues at the surgery site. It is also normal to have some discoloration of the tissues around the surgical site. This too will fade with time. You may notice some slight bleeding at the surgery site after treatment. You may use the provided gauze to help clot this minor bleeding. Minimal talking and activity will help keep these symptoms to a minimum.
- Mouth Rinses: Do not rinse your mouth for the remainder of the day after your surgery. Begin rinsing the following day. There are two different mouth rinses that can be used to help keep the tissues at the surgery site clean.
- Peridex: This mouth rinse may be prescribed to you by your treating doctor. Use this rinse once the morning of the surgery before you come in for your appointment. The day after the treatment, begin rinsing twice a day or as prescribed.
- Salt Water: Warm salt water may also be used to gently rinse your mouth after meals. (1 teaspoon salt in a glass of warm water)
- Packing: Packing is a periodontal dressing that is placed on top of the gum tissue at the surgical site. It has the consistency and appearance of bubble gum. Not all patients will need this dressing. If the packing is placed at the surgical site, it will remain there for 3 to 7 days. It acts as a protective covering and will come off on its own. Do not be alarmed when it begins to come off.
- Brushing: Avoid brushing at the surgical site for the first 24 hours. By the next day, if it is not too uncomfortable, you may begin gentle brushing at the site. By a week after treatment, you should be able to become more aggressive with your brushing. You may notice some slight gum bleeding as you get more aggressive, but this will lessen with time.
- Call: Do not hesitate to call the office if you have any questions about unusual bleeding or severe pain. In case of emergency, you can reach the Dr. Hertzberg at (814) 231-7668 or an emergency number will be given.

