Procedures
Frequently Asked Questions
- Will I feel pain during or after root canal treatment?
- Will my tooth need any special care or additional treatment after the root canal is complete?
- What causes an endodontically treated tooth to need additional treatment?
- Can all teeth be treated endodontically?
- What are the alternatives to endodontic treatment?
- What are the common symptoms a patient may experience if they have a tooth that needs endodontic treatment?
- My dentists told me I need a root canal, but I have no symptoms. Why?
- My dentist told me that I might have a cracked or fractured tooth. What should I know about this?
- Will antibiotics take care of my tooth?
- Do I need the pulp tissues of my tooth that will be removed in root canal treatment?
- How long will it take to do a root canal on my tooth?
- Will I be able to drive and go back to work after my root canal treatment?
- What if I need to talk to my endodontist after working hours?
Will I feel pain during or after root canal treatment?
Many endodontic procedures are performed to relieve the pain of toothaches caused by pulp inflammation or infection. With modern techniques and anesthetics, most patients report that they are comfortable during the procedure. For the first few days after treatment, your tooth may feel sensitive, especially if there was pain or infection before the procedure. This discomfort can be relieved with over the counter or prescription medications. Follow your endodontist’s instructions carefully. Your tooth may continue to feel slightly different from your other teeth for some time after your endodontic treatment is completed. However, if you have severe pain or pressure or pain that lasts more than a few days, call your endodontist.
Will my tooth need any special care or additional treatment after the root canal is complete?
You should not chew or bite on the treated tooth until you have had it restored by your dentist. The un-restored tooth is susceptible to fracture, so you should see your dentist for a full restoration as soon as possible. Otherwise, you need only practice good oral hygiene, including brushing, flossing, and regular checkups and cleanings. Most endodontically treated teeth last as long as other natural teeth. In a few cases, a tooth that has undergone endodontic treatment fails to heal or the pain continues. Occasionally, the tooth may become painful or diseased months or even years after successful treatment. Often when this happens another endodontic procedure can save the tooth.
What causes an endodontically treated tooth to need additional treatment?
New trauma, deep decay, or a loose, cracked or broken filling can cause new infection in your tooth. In some cases, the endodontist may discover very narrow or curved canals that could not be treated during the initial procedure.
Can all teeth be treated endodontically?
Most teeth can be treated. Occasionally, a tooth can’t be saved because the root canals are not accessible, the root is severely fractured, the tooth doesn’t have adequate bone support, or the tooth cannot be restored. However, advances in endodontics are making it possible to save teeth that even a few years ago would have been lost. And, when endodontic treatment is not effective, endodontic surgery may be able to save the tooth.
What are the alternatives to endodontic treatment?
When the pulp of a tooth is damaged, the only alternative to endodontic treatment is extraction of the tooth. To restore chewing function and to prevent adjacent teeth from shifting, the extracted tooth must be replaced with an implant or a bridge. This requires surgery or dental procedures on adjacent healthy teeth and can be far more costly and time-consuming than endodontic treatment and restoration of the natural tooth.
What are the common symptoms a patient may experience if they have a tooth that needs endodontic treatment?
- Temperature sensitivity: When the nerves of the tooth’s pulp chamber become inflamed and/or infected, prolonged sensitivity to cold and heat will begin. Typically, cold sensitivity will be the first symptom a patient will notice. This indicates that a large set of nerves, called the A-fibers, have become inflamed or irritated and as a result, respond to cold at a more heightened level than the nerves in other teeth. Lingering Cold and Heat sensitivity will become more evident as the inflammation reaches the C-fibers, a smaller set of nerves that lie deeper in the pulp chamber. When these nerves become irritated, patients will notice that placing cold or heat on the tooth makes that tooth or that region of the mouth ache for prolonged periods of time.
- Biting/Chewing sensitivity: The pulp extends from the crown of the tooth to the tip or the roots where it connects to the ligament surrounding the root. Once the pulp becomes inflamed, this inflammation can travel to the ligament that surrounds the root. Inflammation in this area can create pressure and may slightly elevate the tooth out of it’s natural socket, causing tenderness to biting and chewing With time, the pulp and inflamed ligament can become infected. This infection eventually destroys the pulp. The byproducts of the pulp destruction along with the infection exit the tooth and break down the ligament and slowly dissolves the jawbone surrounding the root. Once bone loss begins, an abscess is formed. As a tooth reaches this state patients may also complain of spontaneous diffused pain, along with biting/chewing sensitivity in the surrounding regions of this tooth. This is a result of the developing pressure caused by the infection with in the bone.
- Swelling: As an abscess grows, more and more bone loss occurs. Eventually, if no antibiotics or treatments are started, the abscess reaches the gum tissues surrounding the tooth. These tissues become an outlet for the infection and a pocket between the bone and tissue develops. This is when patients begin to notice swelling. Occasionally, instead of a pocket, the infection will create an exit out of the tissues. This usually appears as a small bump or pimple that is used as a drainage site for the infection. Patients that have these typically have very few symptoms because the pressure is relieved by the drainage, however, foul breath and a bad taste are commonly noticed with these cases.
My dentists told me I need a root canal, but I have no symptoms. Why?
Occasionally, root canal therapy is recommended for a tooth that may not be giving a patient any problems. There are a few different cases in which this is true. If your dentist has seen that your tooth has developed an abscess on an x-ray, he/she will recommend a root canal even if you have no symptoms. An abscess indicates that the pulp has been destroyed and that bone loss is occurring. Patients will have no symptoms in this situation because the nerves in the tooth are dead and, the bone that is being dissolved is making room for the infection and very little pressure is exerted on the tooth. Patients that have deep decay/cavity in a tooth may be candidates for needing a root canal if this decay/cavity reaches the pulp chamber. To remove this decay/cavity, your dentist will have to work in the pulp chamber. The bacteria associated with the decay/cavity along with the restoration work needed, will expose and damage the pulp tissues. This damage requires endodontic treatment so future symptoms do not develop.
My dentist told me that I might have a cracked or fractured tooth. What should I know about this?
Cracked teeth show a variety of symptoms, including erratic pain when chewing, possibly with release of biting pressure, or pain when your tooth is exposed to temperature extremes. In many cases, the pain may come and go, and dentists may have difficulty locating which tooth is causing the discomfort. When the outer hard tissues of the tooth are cracked, chewing can cause movement of the pieces, and the pulp can become irritated. When biting pressure is released, the crack can close quickly, resulting in a momentary, sharp pain. Irritation of the dental pulp can be repeated many times by chewing. Eventually, the pulp will become damaged to the point that it can no longer heal itself. Extensive cracks can lead to infection of the pulp tissue, which can spread to the bone and gum tissue surrounding the tooth. Unlike a broken bone, the fracture in a cracked tooth will never heal. In spite of treatment, some cracks may continue to progress and separate, resulting in loss of the tooth. Placement of a crown on a cracked tooth provides maximum protection but does not guarantee success in all cases. The treatment you receive for your cracked tooth is important because it will relieve pain and reduce the likelihood that the crack will worsen. Once treated, most cracked teeth continue to function and provide years of comfortable chewing. Talk to your dentist/endodontist about your particular diagnosis and treatment recommendations. There are many different types of cracked teeth. The treatment and outcome for your tooth depends on the type, location, and severity of the crack.
1. Craze lines:
Craze lines are tiny cracks that affect only the outer enamel. These cracks are extremely common in adult teeth. Craze lines are very shallow, cause no pain, and are of no concern beyond appearances.
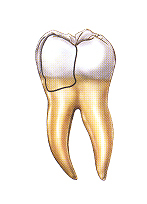
2. Fractured cusp:
When a cusp (the pointed part of the chewing surface) becomes weakened, a fracture sometimes results. The weakened cusp may break off by itself or may have to be removed by the dentist. When this happens, the pain will usually be relieved. A fractured cusp rarely damages the pulp, so root canal treatment is seldom needed. The tooth will usually be restored by your dentist with a full crown.
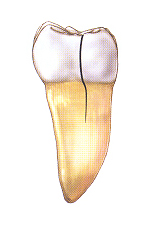
3. Cracked tooth:
This crack extends from the chewing surface of the tooth vertically towards the root. Sometimes the crack may extend below the gum line, and in severe instances, into the root. A cracked tooth is not completely separated into two distinct segments. Because of the position of the crack, damage to the pulp is common. Root canal treatment is frequently needed to treat the injured pulp. Your dentist will then restore your tooth with a full crown to bind and protect the cracked tooth. Early diagnosis is important. Even with high magnification and special lighting, it is sometimes difficult to determine the extent of a crack. A cracked tooth that is not treated will progressively worsen, eventually resulting in the loss of the tooth. Early diagnosis and treatment are essential in saving these teeth.
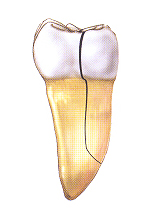
4. Split tooth:
A split tooth is often the result of the long-term progression of a cracked tooth. The split tooth is identified by a crack with distinct segments that can be separated. A split tooth can never be saved intact. The position and extent of the crack, however, will determine whether any portion of the tooth can be saved. In rare instances, endodontic treatment and a crown or other restoration by your dentist may be used to save a portion of the tooth.
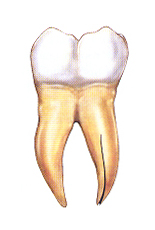
5. Vertical root fracture:
Vertical root fractures are cracks that begin in the root of the tooth and extend toward the chewing surface. They often show minimal signs and symptoms and may therefore go unnoticed for some time. Vertical root fractures are often discovered when the surrounding bone and gum become infected. Treatment usually involves extraction of the tooth. However, endodontic surgery is sometimes appropriate if a portion of the tooth can be saved by removal of the fractured root.
Will antibiotics take care of my tooth?
If the pulp is already inflamed/infected to the point that it cannot repair itself, antibiotics will not repair the situation. Once pulp damage has begun in the tooth, the blood vessel supply to the tooth also breaks down. This eliminates the body’s route into the tooth. Therefore antibiotics can be carried by the body to the surrounding regions of the tooth, however cannot be used to remove the infection inside the tooth. Often times, symptoms of pressure and biting /chewing sensitivity are calmed by the antibiotics as the inflammation/abscess around the tooth are reached. Once a patient finishes the antibiotics, the infection inside the pulp, continues to exit and build around the roots again, causing symptoms to redevelop. The time period of symptoms redeveloping can be day or even months.
Do I need the pulp tissues of my tooth that will be removed in root canal treatment?
The pulp contains blood vessels, nerves and connective tissue. During development of the tooth, these tissues create the surrounding hard tissues of the tooth. After growth and development, the tooth is fully mature and it can survive without the pulp, because the tooth continues to be nourished by the tissues surrounding it.
How long will it take to do a root canal on my tooth?
Keeping in mind that every case is slightly different from the next, a root canal generally takes 30minutes to 1 hour. Almost all treatments are completed in one visit. Chronic cases, in which an abscess has developed, will typically be treated in two visits. During the first visit, a medication called calcium hydroxide will be placed in the cleaned pulped spaces and allowed to set for one week. This medication will help in calming the infection and will be removed at the second appointment when the root canal is completed. Occasionally, the pulp spaces will be difficult to find or clean out if the spaces have become calcified or if a restorative material is blocking the spaces. These cases may require additional visits.
Will I be able to drive and go back to work after my root canal treatment?
Yes. A local anesthetic is used for root canal treatment just like it is used for your general dental work, like fillings and crowns. When you leave the office, you will be numb for 1 to 3 hours. Going back to your daily activities should be of no concern. Please note that if you are having a surgical procedure done in our office you should speak to your endodontist about post-operative instructions.
What if I need to talk to my endodontist after working hours?
We understand that having endodontic treatment can be new or different for each patient. It is quite common and expected for each patient to have many questions and concerns. If you have questions that were not answered while in our office or need to discuss questionable symptoms with Dr. Gillen, he will provide you with his cell phone number after your procedure so he can be reached after hours.

